On the last day of National Sun Awareness week, London Plastic Surgeon Apul Parikh explains to Safety in Beauty readers about the stark reality of excessive exposure to Ultra Violet Rays from the sun and sun beds…
“How many of us living in the UK are aware of the National Sun Awareness (NSA) week? How many of us were aware that this year it ran from the 9th to the 15th of May? I am confident that the vast majority of us (Healthcare professionals as well as the lay public) were blissfully unaware of this! The campaign was launched in 2000 by the British Association of Dermatology (BAD). It aims to create awareness about skin cancer and teaches people about the dangers of sunburn and excessive tanning.
We are all aware that excessive exposure to Ultra Violet Rays (UVR,) is the main causative factor in developing skin cancer. In fact, 80% of malignant melanomas (MM) are linked to exposure to UVR from the sun as well as sunbeds. At present, skin cancer is a sizeable problem in the UK; unfortunately it is rapidly increasing in incidence, and is poised to become an even more severe predicament. The incidence of MM in 2001 was 12/100,000. By 2011, it had soared to 17.6/100,000. Over the last decade, MM was the second fastest growing cancer in males and females, with incidence rates rising by 57% and 39% respectively. In the UK, 2 young adults (15-34 years old) die from MM every day2. With soaring numbers of package holidays in the sun, and the explosion in sunbed usage, deaths from MM are predicted to escalate over the next two decades. Are we doing enough to combat skin cancer?
In 1980, Cancer Council Australia launched what is now generally regarded as one of the most successful public health campaigns to date. “Slip! Slop! Slap! Slip on a shirt, slop on sunscreen and slap on a hat. Slip!Slop!Slap! You can stop skin cancer”, went the jingle. Over the next few years, variations of the Slip!Slap!Slop! scheme could be found in newspapers, on the radio, on national television, as well as billboards in most public places. Public warnings were issued on days when the UV index was raised, advising the population to apply sun block and seek shade. In addition to this, a national education programme was launched in nurseries along with schools. Large scale programmes were also launched to increase the proficiency of General Practitioners to diagnose skin cancers, and educate lay persons on how to avoid sun damage. We are now 36 years from the original campaign launch and only recently have studies in Australia confirmed a decline MM incidence rates in those under the age of 45.
Cancer Research UK predicts a decline in mortality rates for most cancers over the next two decades. However, in the UK, MM is one of the few cancers that is predicted to increase exponentially over this time period. The evidence, according to Cancer Research UK, overwhelmingly suggests that the vast majority of skin cancers are preventable. The key lies in educating the masses about sun protection.
The UK Sunbeds Regulation Act of 2010, banned sunbeds in those under the age of 18; I propose that we take this a step further, and push for a complete ban of all sunbeds. What is also needed is a sustained, multi-faceted national campaign to the extent that the Australians have demonstrated. For all we know, the benefits of such a multi pronged assault on skin cancer may not become evident in the UK for 30 years”.
Tips on spotting melanoma by NHS website
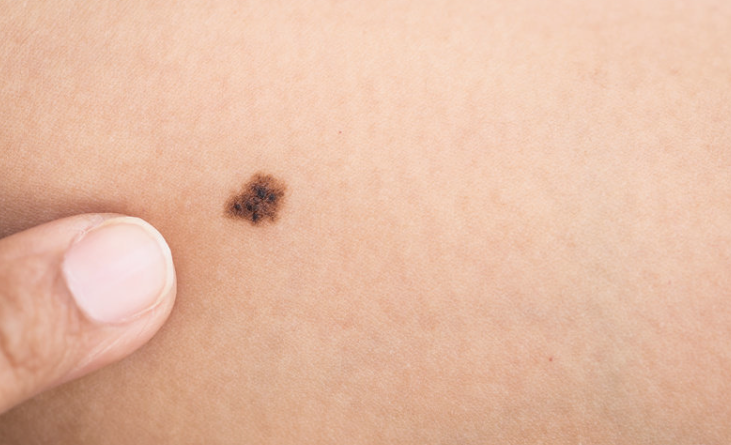
The first sign of a melanoma is often a new mole or a change in the appearance of an existing mole.
Normal moles are usually round or oval, with a smooth edge, and no bigger than 6mm (1/4 inch) in diameter.
See your GP as soon as possible if you notice changes in a mole, freckle or patch of skin, especially if the changes happen over a few weeks or months.
Signs to look out for include a mole that is:
getting bigger
changing shape
changing colour
bleeding or becoming crusty
itchy or painful
A helpful way to tell the difference between a normal mole and a melanoma is the ABCDE checklist:
Asymmetrical – melanomas have two very different halves and are an irregular shape.
Border – melanomas have a notched or ragged border.
Colours – melanomas will be a mix of two or more colours.
Diameter – melanomas are larger than 6mm (1/4 inch) in diameter.
Enlargement or elevation – a mole that changes size over time is more likely to be a melanoma.
Melanomas can appear anywhere on your body, but they most commonly appear on the back, legs, arms and face. They may sometimes develop underneath a nail.
In rare cases, melanoma can develop in the eye. Noticing a dark spot or changes in vision can be signs, although it is more likely to be diagnosed during a routine eye examination.
Want to know more?
Cancer Research UK: Melanoma symptoms.
Article By: Dr Apul Parikh – Safety in Beauty Campaign Expert Panel Advisor
Apul Parikh trained in plastic surgery at most of the leading centres in UK, Europe and the USA.
After completing the European Board of Plastic Surgery (EBOPRAS), he moved into the aesthetic field and works in Harley Street.
He has always had a keen interest in teaching and training. He is currently a cosmetic tutor at the RSM, the RCGP and at MATA courses.